Following on from the multi-award winning Unofficial Guide to Radiology, the Unofficial Guide team return with a practical work book on abdominal X-rays interpretation, giving you all the practice you need to master this vital skill.
Despite its universal importance, X-ray interpretation is often an overlooked subject in the medical school curriculum, making it difficult and daunting for many medical students and junior doctors.
The Unofficial Guide to Radiology: 100 Practice Abdominal X-Rays, with Full Colour Annotations and Full X-Ray Reports aims to help address this. This follow-up textbook, specifically designed for medical students, radiographers, physician’s associates, and junior doctors, builds upon these foundations, providing readers with the opportunity to practice and consolidate their abdominal X-ray assessment and presenting skills.
Key Features
The Unofficial Guide to Radiology: 100 Practice Abdominal X-Rays is an invaluable resource for anyone hoping to gain a practical understanding and a wealth of experience of orthopaedic X-rays and their interpretation in a concise, student-focused manner.

Daniel Weinberg
MBChB (Hons) MPhil
Co-Author
A good starting point is “The Unofficial Guide to Medicine” facebook page, an active forum for medical education. Please get in touch and be part of the medical education project.
100 Abdominal X-rays: Reported and Annotated JUST LIKE THIS
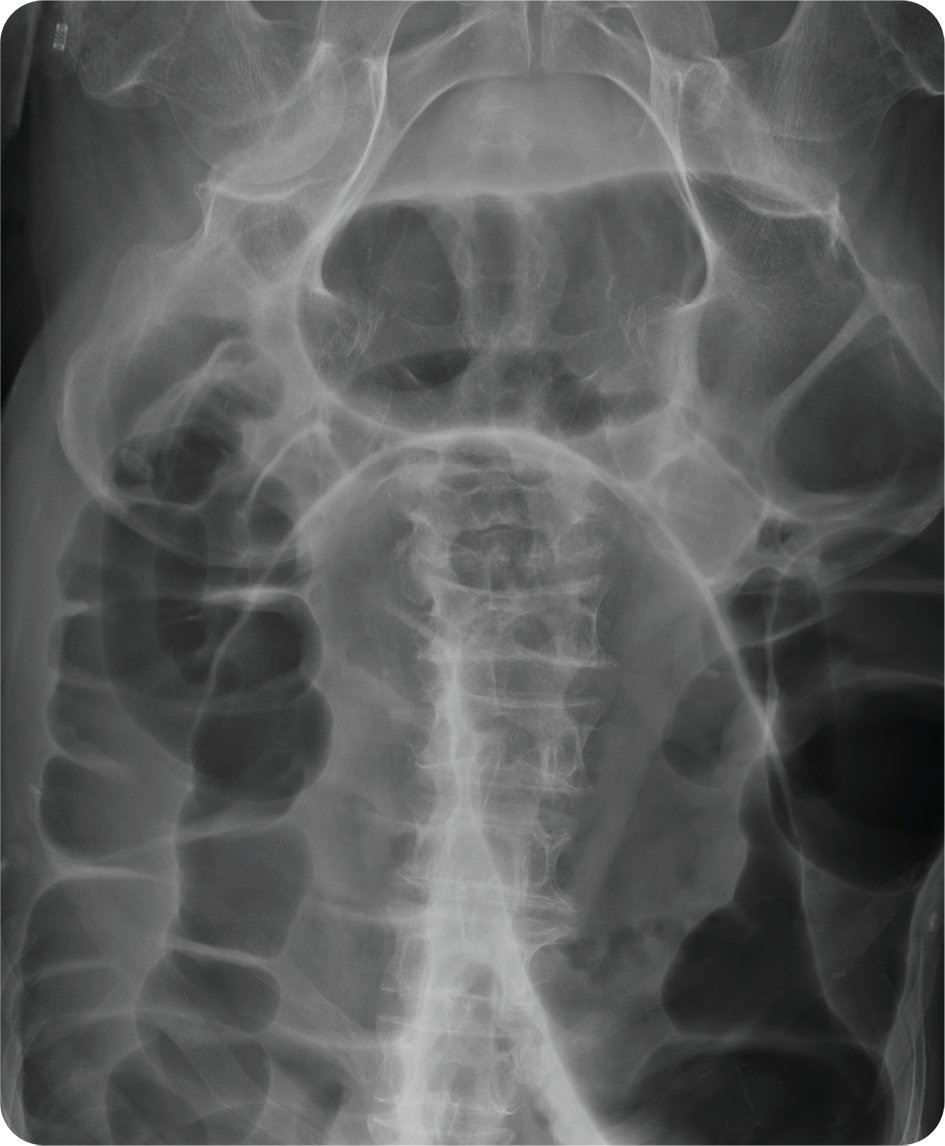
A 45 year old male presents to ED with worsening abdominal distension. He has not passed flatus or opened his bowels for over 48 hours. He has no significant past medical history. On examination, he has saturations of 97% in room air and a temperature of 37.6°C. His HR is 94 bpm, RR is 20 and blood pressure is 134/92 mmHg. The abdomen is rigid and there is generalised tenderness with tinkling bowel sounds. Urine dipstick is unremarkable.
An abdominal X-ray is requested to assess for possible bowel obstruction.
Can you report the X-ray and put in place a management plan?
Turning over the page reveals a full on-image colour annotated X-ray, along with the report, detailing everything you should be expected to see on the X-ray.
Full Report Covering Every Detail Of The X-Ray You Need To Know
Patient ID: Anonymous.
Projection: AP Supine.
Rotation: Adequate.
Penetration: Adequate – the spinous processes are visible.
Coverage: Inadequate – the anterior ribs have not been included.
BOWEL GAS PATTERN
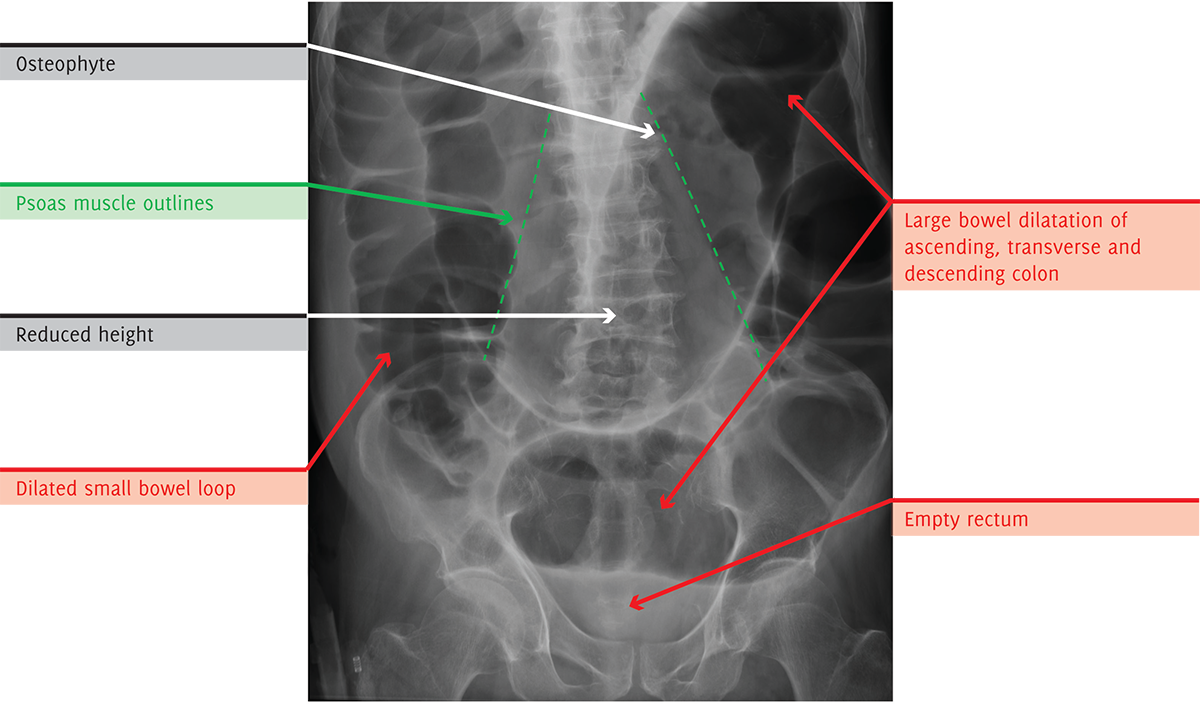
There are multiple loops of dilated bowel seen in the abdomen demonstrating haustra, in keeping with large bowel obstruction. A dilated small bowel loop is visible in the right lower quadrant.
Bowel gas is not seen in the rectum.
BOWEL WALL
There is no evidence of mural thickening or intramural gas within the large or small bowel.
PNEUMOPERITONEUM
There is no evidence of free intra-abdominal gas.
SOLID ORGANS
The solid organ contours are within normal limits with no solid organ calcification.
VASCULAR
No abnormal vascular calcification.
BONES
There are degenerative changes in the lumbar spine with lateral osteophytes at L1/2 and a mild scoliosis convex to the left at L4/L5. The L3 and L4 vertebral bodies have reduced height with concave endplates, in keeping with endplate fractures of indeterminate age.
SOFT TISSUES
The psoas muscle outline is visible bilaterally.
The extra-abdominal soft tissues are unremarkable.
OTHER
There are no radiopaque foreign bodies.
There are no vascular lines, drains or surgical clips.
REVIEW AREAS
Gallstones / Renal calculi: No radiopaque calculi.
Lung bases: Not fully included.
Spine: Degenerative changes and endplate fractures as described.
Femoral heads: Normal.
Fully Annotated X-Ray, With On Image, Colour Labeling For Unbeatable Clarity
SUMMARY, INVESTIGATIONS & MANAGEMENT
This X-ray demonstrates multiple loops of dilated bowel seen within the abdomen demonstrating haustra, in keeping with large bowel obstruction, as well as a loop of dilated small bowel. The absence of gas in the small intestine indicates a competent ileo-caecal valve creating a closed-loop obstruction. The absence of bowel gas in the rectum suggests a distal obstructing point. Given the absence of previous abdominal or pelvic surgery, findings may be secondary to a benign or malignant stricture. Vertebral endplate fractures of indeterminate age are also noted, which may be related to malignancy.
The patient should be resuscitated using an ABCDE approach. Adequate analgesia and hydration should be provided.
The patient should be kept NBM and an NG tube inserted on free drainage. IV fluids should be commenced.
Urgent bloods should be taken, including FBC, U&Es, CRP, LFTs, coagulation, blood gas, and group and save.
The general surgical team should be contacted urgently and a CT scan of the abdomen/pelvis with IV contrast should be considered for better visualisation of the anatomy and further assessment. With regard to the bony changes, further history should be taken, and previous images reviewed.
Contact Us
Are you a medical trainee, a student, a doctor or medical professional?
We’d love to hear from you for feedback or if you would like to contribute towards the Unoffical Guide to Medicine series.